
There are about 1.5 to 2 million stillbirths every year happening in India. About 40% happens during delivery. So delivery should be done at a proper health care facility not at home or under any quacks. Proper regular checkups and also preconception counseling to be done so that stillbirth can be avoided (1).
In this article we are here to discuss in detail about the risk factors, causes, diagnosis, symptoms and how to manage if there is stillbirth. The prevention of stillbirth has also been discussed in this article.
What is a Stillbirth?
Intrauterine fetal death or stillbirth is a delivery of the baby after the period of viability with no signs of life after 24 weeks of gestation. It is around 7.5 per 1000 births in the USA and around 35 per 1000 births in India. (2)
When a woman experiences stillbirth during pregnancy or at childbirth it is not sufficiently addressed in the global platform. There should be more national and international agendas which educate the people about stillbirth, its causes, risk factors and its effects over mental health. (3)
Types of Stillbirth

Generally stillbirth is said after the period of gestation crosses 24 weeks. But there are 3 types of still births which are known. They are-(4)
- Early stillbirth- when the fetus dies between 20 and 26 weeks.
- Late stillbirth- when the fetus dies between 26 to 37 weeks
- Term stillbirth- when the fetus dies above 37 weeks
Who Is At The Risk of Stillbirth?
Stillbirth can happen anytime in any pregnancy, sometimes it is unavoidable. But proper diet, weight, systemic disease check should be maintained to avoid it. The risk includes-(5)
- Age. Stillbirth is commonly seen in teenage mothers and older than 35 years.
- Systemic disease is another risk. Stillbirth is seen as more common if the mother is suffering from diabetes, hypertension, thyroid disorder, renal disease, or heart disease.
- Multiple pregnancy like twins or triplets are more at risk.
- Previous pregnancy complication can cause complication in present pregnancy.
- Substance abuse like tobacco, alcohol, recreational drugs.
- Stress during pregnancy can also cause stillbirth.
- If regular antenatal check ups not done then at term there are risk of stillbirth.
Causes of Stillbirth

There are various causes that affect the fetus which in turn occurs into stillbirth. Stillbirth can be avoided if the causes are known beforehand so the couple can undergo preconception counseling and treatment if there are causes found. It is divided into 4 parts. They are as follows (6)
FETAL CAUSE- around 25-40%, most common
- Congenital malformations- neural tube defects, hydrocephalus, congenital heart disease
- Isoimmunisation due to negative blood group
- Infection- congenital syphilis, cytomegalovirus, toxoplasmosis, parvovirus, rubella, varicella
- Non immune hydrops
PLACENTAL CAUSE- around 15-25% (7)
- Placenta previa, placental abruption
- Placenta and cord abnormalities
- Chorioamnionitis
- Intrapartum asphyxia
- Fetomaternal hemorrhage
- Twin to twin transfusion syndrome
- Excessive coffee intake
MATERNAL CAUSE – around 5-10%
- Hypertensive disorders
- Diabetes mellitus
- Heart and renal disease
- APLA syndrome
- Obstetric cholestasis
- Post term pregnancy
- Hyperpyrexia
- Trauma, sepsis, acidosis
- Abnormal labor, uterine rupture.
UNEXPLAINED CAUSE – around 25- 35%
Sometimes there are instances when every test comes normal but still there is still stillbirth. This is known as unexplained causes which are unavoidable.
Symptoms of Stillbirth

Sometimes there are no symptoms of fetal death; it is incidentally identified when the mother comes for regular antenatal checkup.
But more than 50% of the cases have complaints of decreased fetal movement or no fetal movements. It can also be associated with pain in the abdomen with bleeding per vaginum.(8)
The confirmation of stillbirth is mainly done by the ultrasound of the pregnant women and also by the straight x-ray of the abdomen. But if the above mentioned symptoms are present then immediate consultation with the doctor rather than waiting at home is advised.
How is Stillbirth Diagnosed ?
Repeated examination is often necessary to confirm the diagnosis of intrauterine fetal death. There are some signs which are subtle but present. There are regression of pregnancy like breast changes following the death of a fetus. (9)
There are certain abdominal changes which can be seen. They are-
- Decrease in fundal height
- The uterus can also become flaccid
- Braxton’s contractions are not felt easily
- Fetal movements absent during examination
- Fetal heart sound not heard on stethoscope
- Egg shell crackling feeling of fetal head appears after many days of fetal death
The mother can also complain of decreased or absent fetal movement.
Investigations which can detect fetal death are-
- Ultrasound – No fetal heart, no fetal movement, scalp edema, collapsed cranial bones, fetal hydrops, etc can be detected in ultrasound
- Straight x ray abdomen – There are certain signs that can be seen:
Spalding sign, halo sign, ball’s sign, robert’s sign, concertina effect.
How Is Labor Induced For A Still-born Baby?

Proper counseling to the patient and the relatives to be done before doing any procedure. The family members, mainly the mother, will be upset after hearing the news, so the doctor should be gentle in explaining what is to be done next (10).
The labor should be induced by following methods-
- Prostaglandins- If the cervix is unfavorable by vaginal examination then prostaglandin E2 gel vaginally or intracervical is given and repeated after 6 hours. Sometimes prostaglandin E1(misoprostol) 50mcg can be given orally or vaginally and repeated after 6 hours.
- Oxytocin Infusion- If the cervix is favorable than initially 5 to 10 units of oxytocin in 500ml ringer lactate solution starts intravenously and the dose of oxytocin is escalated.
C section in stillbirth is not generally done. But if a strict obstetric indication is present like major degree of placenta previa, previous 2/3 c section, transverse lie then c section is done. Without proper indication mother should not go through more pain of c section apart from the pain she is already going through.(11)
Dilation And Evacuation (D&E) Of Dead Fetus
Dilatation and evacuation is done only upto period of gestation 20 weeks. More than 20 weeks of gestation the fetus is big enough and undergoes minilabour. The labor is induced with mifepristone and misoprostol and if all the products of conception are expelled there would be any need for dilation and evacuation.(12)
Sometimes patients do not wish to undergo pain, so they are advised for dilatation and evacuation. Here the patient under mild anesthesia cervix is dilated and the products of conception are evacuated. It is an day care procedure.
How Can I Prevent Chances Of Still-Births?
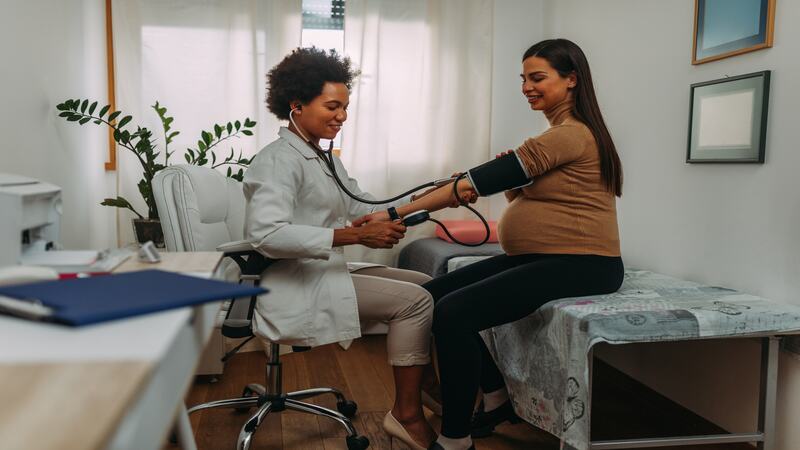
Intrauterine death cannot be totally prevented but there are following guidelines which can help in prevention of intrauterine fetal death. They are (13)
- Preconception counseling should be done to see that the woman should conceive at their optimal health.
- Regular antenatal checkups should be done in the hospital so that any abnormalities can be detected at early stages.
- High risk pregnancies should be detected early and regular monitoring with frequent visits should be done.
- Avoid recreational drugs , tobacco and alcohol use in pregnancy,
- Have a healthy diet with proper nutrition. Junk food, oily and spicy food should be avoided,
- Weight gain should be controlled. In a pregnancy a woman can gain upto 7 to 11 kgs weight.
- Daily fetal kick count chart should be maintained.
- At term sleeping should be on the left lateral side , sleeping on back should be avoided.
- Prevention of infections should be done.
- If there are any abnormal symptoms then healthcare professionals should be informed immediately.
Stillbirth is devastating news not only for the mother but also for the whole family. It might take longer to cope with news of fetal death. Take as much time needed to mourn the dead child. Sometimes when the mother goes into a depressive episode, it is definitely ok to get some help from the professionals, join some support groups and discuss the loss rather than keep everything to herself (14).
Some women are more likely to get stillbirth than the other, so proper preconception checkup to be done with health care professionals. Any problem in the whole pregnancy, immediate consultation with the doctor is needed so to avoid any adverse outcome in the pregnancy. Regular checkups help to avoid stillbirth by early treatment of the problem.
FAQ’s
1. What Are The Side Effects Of A Stillbirth?
The stillbirth comes with its own sets of complications to mother. They are- psychological upset which can lead to depression in future, blood coagulopathies which can affect mothers due to long term stillbirth, infection which is the most common side effect.
2. What Happens To A Mother After Stillbirth?
The mother undergoes an emotional turmoil post the news of stillbirth. As much time as the woman needs to be given to mourn the loss. There can also be post traumatic stress disorder. There should be support from the partner and the family. No one is to blame for the stillbirth.
3. How Long Can A Stillborn Stay In The Womb?
Stillborn as soon as it is detected should be evacuated from the womb by inducing the labor. Sometimes the dead fetus stays for a longer time due to late identification that can cause infection, coagulopathies to the mother.
4. Can I Have A Healthy Baby After Stillbirth?
Yes, a woman can have a normal healthy baby after one stillbirth. But if there is a genetic disorder of the baby or any umbilical cord abnormality is the cause of stillbirth, then there are chances of stillbirth in the next pregnancy.
References
- Frøen, J Frederik et al. The Lancet, Volume 377, Issue 9774, 1353 – 1366 – https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(10)62232-5/abstract#
- Bhutta, Zulfiqar A et al. The Lancet, Volume 377, Issue 9776, 1523 – 1538 – https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(10)62269-6/abstract#
- Lawn, Joy E et al. The Lancet, Volume 377, Issue 9775, 1448 – 1463 – https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(10)62187-3/abstract?rss=yes&TB_iframe=true&width=850&keepThis=true&height=650#
- Goldenberg, Robert L et al. The Lancet, Volume 377, Issue 9779, 1798 – 1805 – https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(10)62235-0/abstract#
- Lawn, Joy EFlenady, Vicki et al. The Lancet, Volume 387, Issue 10018, 587 – 603 – https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(15)00837-5/abstract?code=lancet-site&rss=yes=#
- HE Reinebrant, SH Leisher, M Coory, S Henry, AM Wojcieszek, G Gardener, R Lourie, D Ellwood, Z Teoh, E Allanson, H Blencowe, ES Draper, JJ Erwich, JF Frøen, J Gardosi, K Gold, S Gordijn, A Gordon, AEP Heazell, TY Khong, F Korteweg, JE Lawn, EM McClure, J Oats, R Pattinson, K Pettersson, D Siassakos, RM Silver, GCS Smith, Ö Tunçalp, V Flenady – https://obgyn.onlinelibrary.wiley.com/doi/full/10.1111/1471-0528.14971#
- Linda Björk Helgadóttir, Gitta Turowski, Finn Egil Skjeldestad, Anne Flem Jacobsen, Per Morten Sandset, Borghild Roald, Eva-Marie Jacobsen – https://obgyn.onlinelibrary.wiley.com/doi/full/10.1111/aogs.12044#
- Page, Jessica M. MD; Christiansen-Lindquist, Lauren PhD, MPH; Thorsten, Vanessa BA; Parker, Corette B. DrPH; Reddy, Uma M. MD, MPH; Dudley, Donald J. MD; Saade, George R. MD; Coustan, Donald MD; Rowland Hogue, Carol J. PhD; Conway, Deborah MD; Bukowski, Radek MD, PhD; Pinar, Halit MD; Heuser, Cara C. MD; Gibbins, Karen J. MD; Goldenberg, Robert L. MD; Silver, Robert M. MD. Diagnostic Tests for Evaluation of Stillbirth: Results From the Stillbirth Collaborative Research Network. Obstetrics & Gynecology 129(4):p 699-706 – https://journals.lww.com/greenjournal/abstract/2017/04000/diagnostic_tests_for_evaluation_of_stillbirth_.16.aspx#
- Haws, R.A., Yakoob, M.Y., Soomro, T. et al. Reducing stillbirths: screening and monitoring during pregnancy and labour. BMC Pregnancy Childbirth 9 (Suppl 1), S5 (2009) – https://link.springer.com/article/10.1186/1471-2393-9-S1-S5#
- Ioannis Tsakiridis ORCID logo , Sonia Giouleka , Apostolos Mamopoulos , Apostolos Athanasiadis and Themistoklis Dagklis ORCID logo EMAIL logo From the journal Journal of Perinatal Medicine – https://www.degruyter.com/document/doi/10.1515/jpm-2021-0403/html#
- Menezes, E.V., Yakoob, M.Y., Soomro, T. et al. Reducing stillbirths: prevention and management of medical disorders and infections during pregnancy. BMC Pregnancy Childbirth 9 (Suppl 1), S4 (2009). – https://link.springer.com/article/10.1186/1471-2393-9-s1-s4#
- Darmstadt, G.L., Yakoob, M.Y., Haws, R.A. et al. Reducing stillbirths: interventions during labour. BMC Pregnancy Childbirth 9 (Suppl 1), S6 (2009). https://doi.org/10.1186/1471-2393-9-S1-S6 – https://link.springer.com/article/10.1186/1471-2393-9-S1-S6#
- Ruth C. Fretts, Etiology and prevention of stillbirth, American Journal of Obstetrics and Gynecology,
Volume 193, Issue 6, 2005, Pages 1923-1935, –
https://www.sciencedirect.com/science/article/abs/pii/S0002937805005119# - McClure, E. M., Saleem, S., Pasha, O., & Goldenberg, R. L. (2009). Stillbirth in developing countries: a review of causes, risk factors and prevention strategies. The Journal of Maternal-Fetal & Neonatal Medicine, 22(3), 183–190. – https://www.tandfonline.com/doi/abs/10.1080/14767050802559129#
