Pelvic Pain During Pregnancy
5 min readWritten by Editorial Team

Pelvic pain or uneasiness around the pelvic region is normal in the course of pregnancy. Considering the fact that the ligaments are stretched, hormone levels are changing, and organs are moving around to make space for the developing womb, experiencing pelvic pain can be expected. However, sometimes this pain could be a warning of some serious issues.

What Is Meant By Pelvic Pain?
Pelvic pain is the pain that is experienced below the belly button, between the hipbones (pelvic bones). The pain can be sharp or mild, can appear and disappear, and can be sudden and intense, depending on the reasons. Generally, pelvic pain is not a reason to panic. A majority of pregnant women experience pelvic pain, sooner or later, inevitably as the pregnancy advances. Most often pelvic pain is experienced during the last trimester as the bones and ligaments shift and stretch to accommodate the fetus and the strain on the pelvic area increases.
How Is Pelvic Pain Different From The Usual Abdominal Pain During Pregnancy?
Sometimes abdominal pain is mistaken as pelvic pain by some women. The abdominal pain that is experienced in the course of pregnancy is usually concentrated in the upper part of the body. Whereas, the pelvic pain happens over the pelvic region. The abdominal pains are less sharp than pelvic pain and remain almost constant irrespective if the expecting mother is lying down or walking. Whereas, the pelvic pain will get sharper and more noticeable during walking, climbing steps, standing on one leg (when wearing pants or panties or while getting in and out of the car etc.) or even tossing and turning in the bed.
What Is Pelvic Girdle Pain (PGP)?
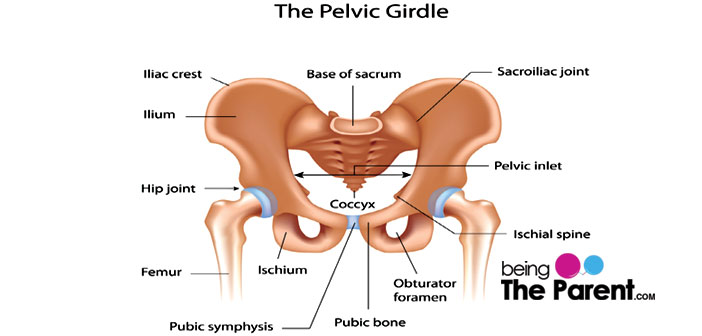
The pelvic girdle is a bony arched structure in the hip area, which bears several bones and joints. Pelvic joint is mainly formed of two curved pubic bones meeting at the joint called the pubic symphysis , hip joint (which bear the weight of the body), and the sacroiliac joint (connecting the sacrum with the pelvis). Any mechanical issues happen to these joints usually leads to pelvic girdle pain (PGP).
There are two types of pelvic girdle pains, SPD (Symphysis pubis dysfunction) and DSP (Diastasis symphysis pubis). Though related to SPD, the DSP is not that common as SPD. DSP refers to a condition in which the pubic symphysis widens too far. An X-ray, ultrasound scan or MRI scan can only diagnose this condition.
What Is Symphysis Pubis Dysfunction SPD?
Symphysis pubis dysfunction (SPD) refers to a condition in which the ligaments that ordinarily keep the pelvic bone in position during pregnancy, turn out to be excessively relaxed and stretchy. This results in the loosening of the pelvic joint (symphysis pubis). It can bring about pain and discomfort around the pelvic region. Around 2% of the expecting mothers are found to experience SPD in the course of pregnancy.
What Causes Symphysis Pubis Dysfunction SPD?
Normally, the muscles and joints of the mother are capable of adapting and adjusting to the changes the pregnancy hormone relaxin induces to the joints. The body automatically takes new postures, which bring about fewer pressures on the joints. SPD happens when the mother’s body fails to adapt to the new changes and affecting the stability of the pelvis, like the joints in the pelvis moving unevenly when you move about. SPD can also happen when one of the pelvic joints does not work properly, causing pain in other joints.
What Are The Symptoms Of Pelvic Girdle Pain?
The severity of the symptoms of pelvic girdle pain varies with the expecting mothers. The symptoms can be either mild or so severe that makes it hard to move about. The symptoms can happen any time during pregnancy, either all of a sudden or progressively. The signs of SPD are:
- Pain in the pubic area
- Pain in the hip area
- Pain in the area where the thigh meets the abdomen
- Difficulty with walking and climbing steps
- Pain across the sides of the lower back
- Pain radiating toward the thighs
- Pain worsens at night making it difficult to getting up and going to the toilet (which are more frequent during the third trimester)
Is Normal Vaginal Birth Possible If The Mother Has SPD?
Numerous women with pelvic pain in pregnancy can have normal vaginal birth. Find birth positions that are the most agreeable for you. Note them down and discuss it with your midwife or doctor. Being in water can reduce the weight on the joints and permit you to move even more effortlessly, so you can also consider having a water birth. You can ask about its probability to your specialist.
Am I At A Risk Of Developing Pelvic Girdle Pain?
The risk factors that make an expecting mother more prone to develop SPD are:
- If the mother has a history of pelvic girdle issues
- If the mother is already experiencing a lower back pain
- If the pelvic girdle is already injured before pregnancy (as a result of an accident)
- If the mother has a history of SPD in the previous pregnancy or pregnancies
- If the job of the mother demands hard physical exertion
- If the mother clings to a poor posture which puts more pressure on the pelvic bone
- If the mother is obese
Regardless of the fact that you do not have one of these risk factors, you can still develop SPD.
What Is The Treatment For Pelvic Girdle Pain?
Physiotherapy is the best method to treat SPD, in light of the fact that, it’s more related to the muscles and bones, than an intense loosening of the joints.
- Manual therapy can ensure the normal movement of the hip, spine, and the joints of the pelvic girdle.Choose a therapist who is considerably experienced in caring for pregnant women
- Exercising in the water is more effective as you can move about without much effort in in water
- A well experienced and trained acupuncturist can help to reduce the pelvic pain in pregnancy safely
- Wearing a pelvic support belt can also help in treating SPD
How Can I Cope With The Pain Of SPD?
You can cope with SPD if you take care of the following:
- Never stand on one leg: Standing on one leg will worsen the SPD pain, and also will increase the pressure on the pelvic girdle. Adapt sitting position while dressing or undressing. While getting in and out of a car try to keep the knees together
- Stay active: Be as active as you can, as far as you are not exceeding your pain threshold. Being active ignoring the pain can worsen the issue. Remember to avoid activities that put the pelvis in uneven position and stop whatever activity you are doing if it causes pain
- Never lift weights: Lifting weights, even if it is your toddler, aggravates the pain. Pushing something like trolleys or anything that is heavy should also be kept off.Carrying anything,even if it will not weigh much, in one hand should also be avoided as it can affect the evenness of pelvic bone
- Sleep in a healthy position: Always sleep on a side with a pillow between the legs. If you have to turn over, always try to keep the knees together. Hold the headrest and press the buttock as you turn
- Don’t cross the legs: Never cross the legs even if you are sitting as it will place the pelvis in uneven position
- Never stand or sit for a long time: Avoid standing for a long time (in queue, or while ironing or cooking) in the same position. Avoid sitting on the floor
- Climb steps one at a time: Climbing steps first with your comparatively healthy leg, followed by the other. Take one-step at a time

Editorial Team,
With a rich experience in pregnancy and parenting, our team of experts create insightful, well-curated, and easy-to-read content for our to-be-parents and parents at all stages of parenting.Read more.
Responses (0)
Want curated content sharply tailored for your exact stage of parenting?
Related articles
Sponsored content
Discover great local businesses around you for your kids.
Get regular updates, great recommendations and other right stuff at the right time.